Too many children in sub-Saharan Africa die each year from typhoid. Left untreated, the disease can cause complications such as intestinal bleeding and holes—perforations—that develop within weeks of infection. These perforations are life-threatening and require immediate surgical care. While typhoid cases have declined significantly in high-income countries, with mortality rates less than 1 percent, an estimated 10.9 million cases occur annually, mostly in low- and middle-income countries.

In low-resource settings where access to clean water, sanitation, and hygiene (WASH), as well as surgical care, may be limited, prevention of typhoid is lifesaving. While improvements to WASH infrastructure and surgical facilities are optimal, they often don’t exist and are costly to implement in many parts of the world. Prevention can decrease deaths and is an important part of a comprehensive approach to typhoid control that includes typhoid conjugate vaccines (TCV), improvements in WASH, and greater access to health care.
A new article in the World Journal of Surgery reviews more than 20 years of typhoid intestinal perforation data from sub-Saharan Africa, where such incidence peaks in children 5 – 9 years of age. The research shows intestinal perforation impacts an estimated 0.8 percent – 39 percent of untreated or improperly treated cases worldwide. Unfortunately, it is highly likely that many children suffering from these perforations die before they ever reach a health care center. This is especially true in medically resource-poor areas where travel to a hospital is often long and difficult, and where the hospitals often lack specialized surgical and postoperative care units.
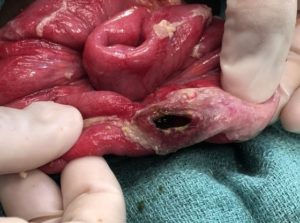
Data on intestinal perforation are limited in sub-Saharan Africa. The data that are available show little improvement in associated deaths during the last 30 years. The continued high mortality rates are attributed to late presentation at the health care center due to delayed or incorrect diagnosis and difficulty finding adequate care, including appropriate antibiotics, in rural areas. Many patients first visited outpatient clinics or traditional healers and arrived at tertiary health care centers (referral hospitals) with conditions requiring attention prior to surgery. This results in a longer duration between when the perforation forms and surgery, which has been shown to increase morbidity and mortality. In addition, the number of perforations present, lack of access to critical care management or an intensive care unit, and inadequate culture data to guide antibiotic therapy contribute to poor outcomes for these patients.
We want to prevent typhoid—the illness causes pain and suffering in addition to economic hardship and educational loss. And, there is increased drug resistance and diagnostic limitations. We are fortunate to have a TCV that is safe and effective for children as young as six months. Prevention, via routine immunization of children with TCV, in conjunction with improved sanitation infrastructure and robust community education on health and proper hygiene practices, is ideal. However, once a child has typhoid, proper interventions to stop disease progression are lifesaving.
It is anticipated that prevention of typhoid, with the help of TCV, will lead to reductions in perforations and associated morbidity and mortality. Unfortunately, WASH improvements and infrastructure strengthening are difficult and expensive to implement in resource-limited settings. Thus, vaccination is that much more important. In sub-Saharan Africa, especially in rural areas, additional research is needed to highlight the burden of typhoid and its complications, and catalyze efforts to properly treat, and prevent, this disease.



