This paper is part of Charting the Course to Meet the Challenges Ahead: Research and Developments on Typhoid and Other Invasive Salmonelloses.
Typhoid remains a real threat in low- and middle-income countries due to the lack of clean water and difficulty accessing healthcare services. School-aged children are disproportionately impacted and accounted for more than 50% of typhoid deaths in 2017. Although blood cultures are the gold standard to diagnose typhoid, many endemic countries are unable to routinely provide these tests due to resource limitations and lack of laboratory capability. As a result, it is difficult to conclusively diagnose typhoid, leading to underreported cases, inadequate or incorrect treatment, and more severe clinical outcomes. Alternative country-level indicators of typhoid burden are essential, especially in the most marginalized settings.
The Severe Typhoid Fever in Africa (SETA) study conducted broad typhoid surveillance from 2016 – 2021. In a newly published sub-study, 608 SETA participants who underwent surgery for suspected non-traumatic intestinal perforation were identified. Of these, 33 tested positive for Salmonella Typhi (S. Typhi) and 214 cases had surgical findings based on operative reports that strongly supported a diagnosis of typhoid intestinal perforation (TIP). These results are consistent with previous studies that found low blood culture positivity in TIP patients, likely due to delayed healthcare seeking and antibiotic use before blood collection.
To further explore the cause of these intestinal perforations, researchers correlated the timing of the cases with positive blood cultures for S. Typhi and found a significant correlation between monthly intestinal perforations and blood culture-confirmed typhoid cases across six African countries: Burkina Faso, Democratic Republic of Congo (DRC), Ethiopia, Ghana, Madagascar, and Nigeria. This correlation remained significant in DRC, Ghana, Nigeria, and Ethiopia, all of which had high burden of disease. Children under 15 were disproportionately impacted by TIP, particularly in countries with higher burden of disease.
How are intestinal perforations and typhoid related?
Due to delayed healthcare access, patients in low- and middle-income countries are more likely to develop severe disease, thus leading to an increased risk of complications, such as TIP. In the operating room, surgeons will see oval anti-mesenteric perforations in the small bowel, which is specific for TIP. During an epidemic in Malawi, an estimated 43% of intestinal perforations were due to typhoid. During a severe outbreak of typhoid in DRC, corresponding regions noted a parallel increase in peritonitis cases. In endemic regions, like Niger, perforation cases vary monthly and parallel the typhoid season, oftentimes spiking during or immediately after the rainy season.
Intestinal perforations: A new data driver
This study supports the notion that intestinal perforation can be used as an indicator of underlying typhoid burden, although extrapolation of TIP occurrence to typhoid incidence needs to be further investigated. Over-reliance on blood culture likely underestimates the true burden of disease, as it does not account for the most severe and prolonged typhoid cases, or the incomplete sensitivity of blood cultures. Non-traumatic intestinal perforations can act as a surrogate in areas where laboratory diagnosis is not available.
Fortunately, a single dose of typhoid conjugate vaccine (TCV) is safe—and approximately 80% effective—for children as young as 6 months of age. Three African countries—Liberia, Malawi, and Zimbabwe—have introduced TCV in their routine immunization schedule. We need more! A lack of data on typhoid burden remains a challenge to the introduction of TCV in many endemic countries. The high burden of disease, outbreaks, and increasing multidrug resistance elevates the urgency to control typhoid. It is imperative that countries gather and assess various data and risk factors to make informed decisions on the introduction of vaccines.
TIP is a commonly seen by surgeons in endemic countries. As a result, typhoid is often diagnosed in the operating room. These data provide a new and essential tool to empower policymakers to make informed decisions regarding TCV introduction. TCV remains an affordable and effective method to reduce the burden of typhoid, particularly for children in the most marginalized regions where blood culture data are lacking.
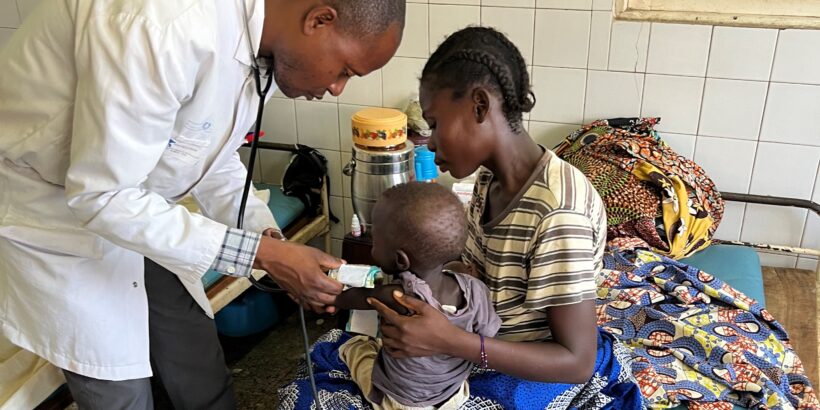
Cover photo: A child being examined during the SETA study. Credit: IVI/Justin Im.