Adjacent to the beautiful tea estates in the highlands west of the Kenyan Rift Valley, sprawls the Microbiology Hub-Kericho (MHK), a state of the art research laboratory established in 2009 by the US Army Medical Research Directorate-Africa (USAMRD-A). The laboratory was launched with a core mission to conduct enteric pathogen surveillance studies at county hospitals under the Department of Emerging Infectious Diseases (DEID) program in Kenya. This was important in enhancing preparedness for emerging infectious diseases so as to protect the health of the public (civilian & military). The MHK occupies more than 11,000 square feet of space with general lab and office space, and four temperature-controlled units. MHK is now well-equipped to provide diagnostic capabilities and microbiology lab support for infectious diseases, including isolation & identification of enteric pathogens, detection and tracking of emerging antibiotic resistance, and outbreak support and response.
The MHK has a well-established network to ensure samples seamlessly make it from patients into the lab. The sentinel site personnel identify and enrol participants at the hospitals/clinic into the studies, collect and prepare the samples, and ship them to the MHK within the expected timeline. At the MHK, there are skilled and knowledgeable personnel who perform everything from simple to very complex analysis to identify pathogens, assess risk, and note any potential outbreak response. On a daily basis, the laboratory buzzes with robust activities to identify pathogens, track diseases, and keep the people of Kenya protected. The lab also performs microscopy to detect parasites and immunological assays in support of vaccine development pipelines. Crucially, once a sample has been analysed, the results are immediately transmitted back to the sentinel site for physicians’ reference.
Diarrheal diseases are common in Kenya, especially in the rural areas where access to clean water is a challenge. Although there are municipal water supplies, most households lack access and so they obtain water from boreholes or rivers and mostly consume it untreated. Defecation in the open, either in the bush or by the roadside is also not unusual. Being infected with an enteric pathogen such as Salmonella is therefore a common encounter. However, the diagnostic activities in most local health facilities in Kenya are limited and it takes several days to receive results from MHK for those whose samples are received, so too many fevers are treated presumptively as malaria, and when symptoms persist, antibiotics are prescribed for suspected typhoid. Additionally, the readily available over-the-counter antibiotics have encouraged self-medication.
Although MHK is well-positioned to confirm cases of typhoid, the reality is that it is a long and expensive process leading to incorrect empirical treatment before a diagnosis is made. Adoption and implementation of the recent WHO recommendation for a prequalified typhoid conjugate vaccine (TCV) has the potential to reduce morbidity and mortality from typhoid in Kenya. By protecting people from typhoid, disease transmission is more limited, drug resistance evolves more slowly, and children miss fewer days of school (and parents off work) while ill with typhoid.
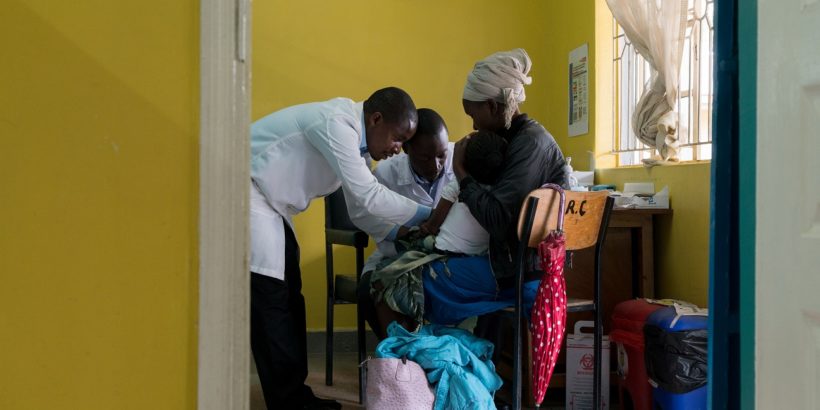
Photo: Sabin Vaccine Institute / Adriane O’Hanesian